The government wants to curb NDIS spending. Here’s how it might succeed
- Written by: Sam Bennett, Disability Program Director, Grattan Institute

Australia’s National Disability Insurance Scheme (NDIS) has grown too big, too fast.
The NDIS is a government-funded program providing support[1] to more than 760,000 disabled Australians[2]. It launched in 2013[3] as a way to make disability support more accessible and equitable.
But public support for the NDIS is faltering. It’s one of the most expensive items in the federal budget, expected to cost taypaxers more than A$50 billion[4] this year. And it’s a flawed system in urgent need of reform.
Reform is coming in May[5], with the federal government aiming to reduce the scheme’s annual growth from 10% to between 5% and 6% in the forthcoming budget.
So is that achievable? And what needs to change?
Ripe for reform
The NDIS was designed to replace an existing disability support system that was underfunded, fragmented and deeply inequitable[6].
In 2011, the Productivity Commission estimated the fully-developed scheme would cost $13.5 billion[7] and would grow between 3% and 6% each year.
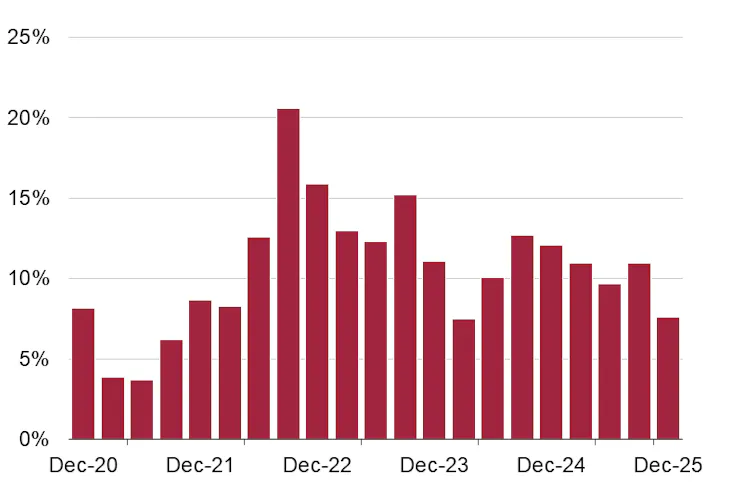
But this year its costs will grow to more than $50 billion[8]. And growth is tracking at over 10% this year so far.
The government is now aiming to curb the annual growth of NDIS expenditure to 5% or 6%[9]. This is not an unreasonable target. Both Medicare and aged care costs are projected to grow[10] within this same range.
But if it’s not careful, the government risks hitting the target while missing the point. Rather than fixing the flaws in the NDIS, tightening at the margins alone may make the scheme worse for Australians with disability that need it most.
Where to start?
One of the clearest flaws is early childhood supports.
When the Productivity Commission first proposed the NDIS in 2011, it estimated how many adults and children would be supported by the scheme. Today, the number of adults on the NDIS is only slightly higher[11] than that original estimate. The number of children, however, is more than double[12].
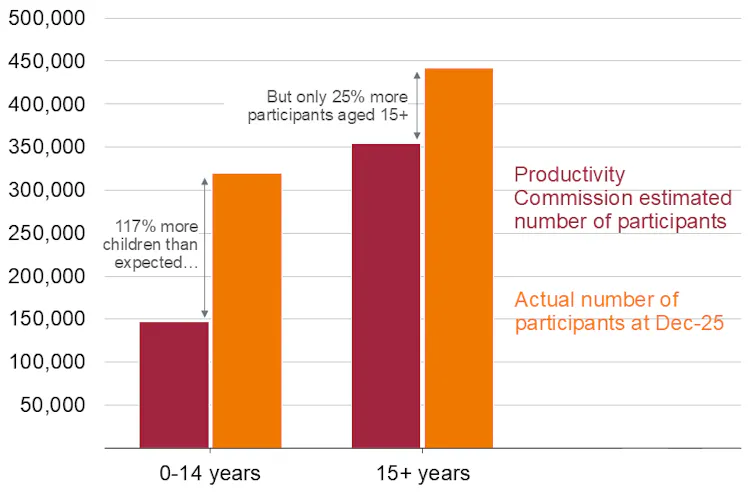
Children with autism or developmental delay make up almost half[13] of all people on the NDIS. In 2025, about 170,000 of these children were receiving early intervention supports, such as speech pathology or occupational therapy.
These supports are delivered through individualised funding. This means each person on the scheme is given a budget with which to purchase their own supports. That’s instead of funding going directly to a service provider.
However, this individualised funding model has its downsides. It has led to a disproportionate focus on therapies delivered in clinical settings[14] rather than supporting children and families in their everyday environments, such as at home or in childcare.
This model has also contributed to an increase in diagnoses. Research suggests during the NDIS rollout, there was a 32% rise[15] in reported diagnoses of child autism compared to rates before the NDIS was introduced.
The government made a major policy misjudgement in including early childhood intervention in the NDIS. It’s a major reason why the cost of the scheme is growing so rapidly.
Instead, we should deliver early childhood intervention supports as a commissioned program. This would involve directly funding service providers to offer evidence-based supports for children in places where they live, learn and play.
The government should expand its Thriving Kids[16] initiative. This new nationwide program aims to support children with developmental delay and/or autism who have low to moderate support needs.
In its current form, Thriving Kids will target children aged eight years and below. But to help curb the growing costs of the NDIS, the government should make this program available to all school-age children. The NDIS should be reserved for children with permanent and significant disabilities.
What else needs to change?
To reach its 5% to 6% growth target, the government should prioritise reform in three other parts of the NDIS.
1. Improving planning
The current way the NDIS builds plans for participants is a major driver of the scheme’s unsustainable growth. The process involves a person requesting support items, and an NDIS planner then determining which ones are “reasonable and necessary” for them.
This is a highly subjective, and often adversarial, process which leads to inconsistency between plans. It also contributes to year-on-year inflation, meaning individual plans cost more.
Importantly, the government’s “new framework planning[17]” approach is a step in the right direction. It aims to make planning clearer and more transparent for NDIS participants. Standardised assessments, which look at a participant’s individual support needs and personal and environmental context, should ensure funding is more fairly distributed, according to need.
However, the government’s proposed rules governing how funds can be spent could deny participants the flexibility to use funds as they need, and require a rethink before they are implemented.
2. Rethinking psychosocial support
To date, the NDIS has failed to provide suitable support to many people with psychosocial disability[18]. This refers to disability arising from significant mental health conditions, such as schizophrenia, major depression or post-traumatic stress disorder, that affects a person’s ability to function.
Current NDIS psychosocial spending is poorly targeted[19]. More than 90% of all government spending in this area funds packages for 66,000 people on the NDIS. Meanwhile, more than 130,000 adults with the greatest support needs miss out entirely.
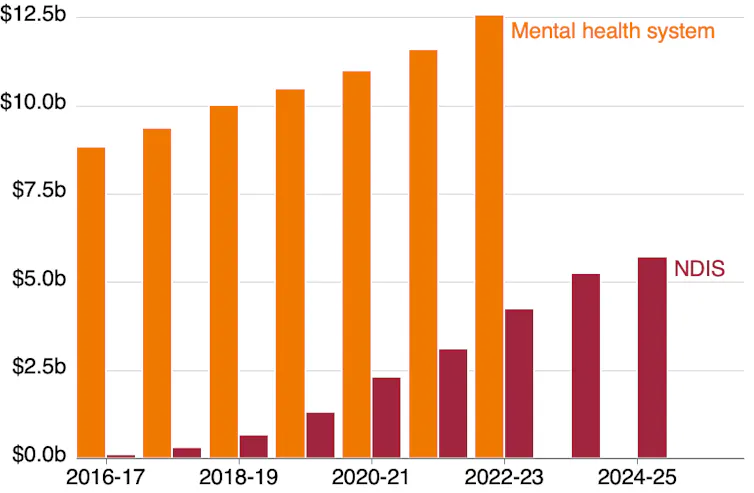
Many of the supports currently funded by the NDIS don’t encourage personal recovery[20], which aims to give participants a sense of independence and purpose. Instead, about 80% of currently-funded supports focus on practical daily tasks, such as cleaning, cooking and transportation. These are important for people with psychosocial disability. However, there’s no evidence funding these supports long-term aids people’s recovery.
Instead, the government should redirect a portion of these funds to a program outside the NDIS[21] that prioritises evidence-based, recovery-oriented supports to reduce demand on the scheme.
3. Better supporting people with the highest needs
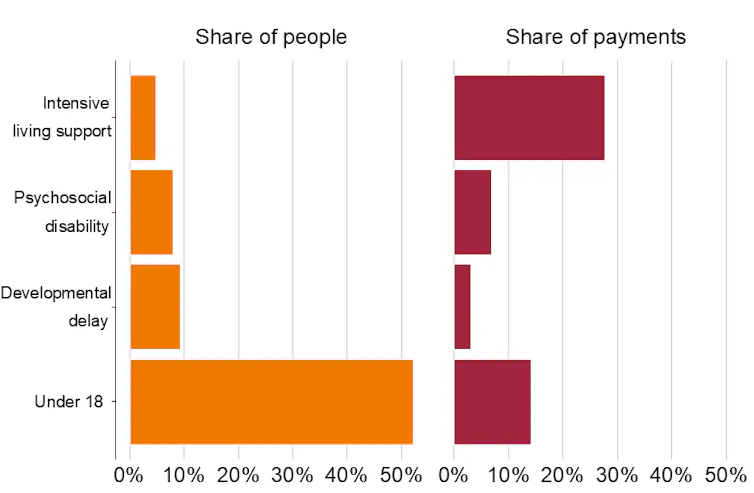
About one-third of NDIS payments go to just 5%[22] of participants. These are people with disability who require the highest level of daily support.
Providing support to these Australians is one of the scheme’s most important responsibilities. However, it’s also where it currently delivers the least value for money.
A major reason is too many participants remain in group homes[23] where they share supports with other disabled people. The Disability Royal Commission raised serious concerns[24] about group homes, with residents frequently experiencing violence, abuse and neglect. They are also expensive, with individual plans including funding for group homes costing an average of $487,300[25] each year.
Thankfully, there are better options. Alternative models, such as living with host families[26] or in home-share arrangements, allow people with disability to live independently in regular homes while still getting the support they need. They often improve participants’ quality of life by increasing their community involvement. And they can also reduce the cost of care by using different types of support, instead of relying solely on paid support workers.
The bottom line
The current NDIS system is financially unsustainable, so the government must act quickly to moderate its growth. But it should do so in a way that makes the scheme work better for the people who need it most. If not, we risk creating an NDIS that costs less, but delivers less too.
References
- ^ providing support (www.health.gov.au)
- ^ 760,000 disabled Australians (www.ndis.gov.au)
- ^ launched in 2013 (www.ndis.gov.au)
- ^ A$50 billion (www.ndis.gov.au)
- ^ in May (www.theage.com.au)
- ^ deeply inequitable (grattan.edu.au)
- ^ $13.5 billion (www.theage.com.au)
- ^ $50 billion (www.ndis.gov.au)
- ^ 5% or 6% (www.smh.com.au)
- ^ projected to grow (budget.gov.au)
- ^ slightly higher (grattan.edu.au)
- ^ more than double (grattan.edu.au)
- ^ almost half (grattan.edu.au)
- ^ clinical settings (www.ndisreview.gov.au)
- ^ 32% rise (grattan.edu.au)
- ^ Thriving Kids (theconversation.com)
- ^ new framework planning (consultations.health.gov.au)
- ^ psychosocial disability (theconversation.com)
- ^ poorly targeted (grattan.edu.au)
- ^ personal recovery (grattan.edu.au)
- ^ outside the NDIS (grattan.edu.au)
- ^ just 5% (grattan.edu.au)
- ^ group homes (disability.royalcommission.gov.au)
- ^ serious concerns (disability.royalcommission.gov.au)
- ^ $487,300 (dataresearch.ndis.gov.au)
- ^ host families (grattan.edu.au)




























