US Black and Latino communities often have low vaccination rates – but blaming vaccine hesitancy misses the mark
- Written by: Elisa J. Sobo, Professor and Chair of Anthropology, San Diego State University
By early July 2021, nearly two-thirds[1] of all U.S. residents 12 years and older had received at least one dose of a COVID-19 vaccine; 55% were fully vaccinated. But uptake varies drastically by region – and it is lower on average among non-white people[2].
Many blame the relatively lower vaccination rates in communities of color[3] on “vaccine hesitancy.” But this label overlooks persistent barriers to access and lumps together the varied reasons people have for refraining from vaccination. It also places all the responsibility for getting vaccinated on individuals. Ultimately, homogenizing peoples’ reasons for not getting vaccinated diverts attention away from social factors[4] that research shows play a critical role in health status and outcomes.
As medical[5] anthropologists[6], we take[7] a more nuanced view. Working together as lead site investigators for CommuniVax[8], a national initiative to improve vaccine equity[9], we and our teams in Alabama, California and Idaho, along with CommuniVax teams elsewhere in the nation, have documented a variety of stances toward vaccination that simply can’t be cast as “hesitant.”
Limited access hampers vaccination rates
People of color have long suffered an array of health inequities[10]. Accordingly, due to a combination of factors[11], these communities have experienced higher hospitalization due to COVID-19, higher disease severity[12] upon admission, higher chances for being placed on breathing support and progression to the intensive care unit, and higher rates of death.
CommuniVax data, including some 200 in-depth interviews within such communities, confirm that overall, those who have directly experienced this kind of COVID-19-related trauma[13], are not hesitant. They dearly want vaccinations. For example, in San Diego’s heavily Latino and very hard-hit “South Region,” COVID-19 vaccine uptake is remarkably high – about 84% as of July 6, 2021[14].
However, vaccine uptake is far from universal in these communities. This is in part due to access issues that go beyond the well documented challenges[15] of transportation, internet access and skills gaps, and a lack of information on how to get vaccinated. For example, some CommuniVax participants had heard of non-resident white people usurping doses that were meant for communities of color. African American participants, in particular, reported feeling that the Johnson & Johnson vaccines promoted in their communities[16] were the least safe and effective.
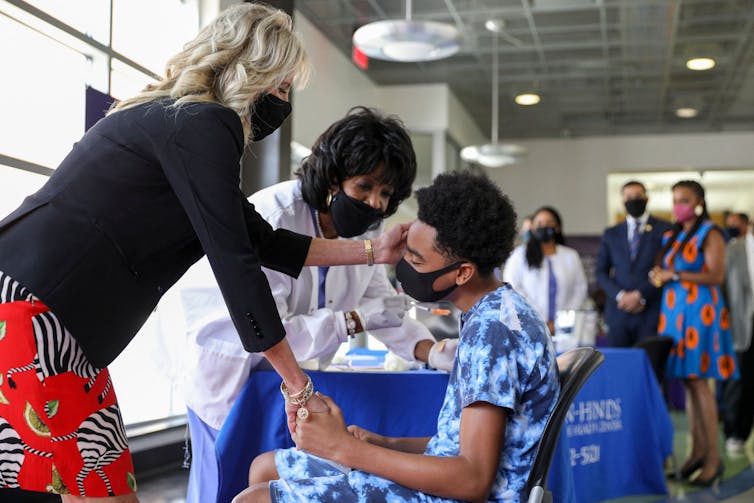 The Biden Administration fell short of its Fourth of July target to have at least one shot to 70% of adults.
Tom Brenner/Pool/AFP via Getty Images[17]
The Biden Administration fell short of its Fourth of July target to have at least one shot to 70% of adults.
Tom Brenner/Pool/AFP via Getty Images[17]
Our participant testimony shows that many unvaccinated people are not “vaccine hesitant” but rather “vaccine impeded.” And exclusion can happen not just in a physical sense; providers’ attitudes towards vaccines matter too[18].
For instance, Donna, a health care worker in Idaho, said, “I chose not to get it because if I were to get sick, I think I would recover mostly or more rapidly.” This kind of attitude by health care providers can have downstream effects[19]. For example, Donna may not encourage vaccination when on duty or to people she knows; some, just observing her choices, may follow suit. Here, what appears as a community’s hesitancy to vaccinate is instead a reflection of vaccine hesitancy within its health care system.
More directly impeded are community members who, like Angela in Idaho, skipped vaccination because she couldn’t risk having a negative reaction that might require intervention. Although a trip to the doctor is a highly unlikely outcome after a vaccine, it remains a concern for some. “My insurance doesn’t cover as much as it possibly, you know, should,” she noted. And we have encountered many reports of undocumented individuals who fear deportation although, according to current laws[20], immigration status should not be questioned in relation to the vaccine.
Christina, in San Diego, illustrates another type of practical barrier. She cannot get vaccinated, she said, because she has no one to care for her babies should she fall ill with side effects. Her husband, similarly, can’t take time off from his job – “It doesn’t work that way.” Likewise, Carlos – who made sure that his centenarian father got vaccinated – says he can’t take the vaccine himself due to his dad’s deep dementia: “If I took my vaccine and I got sick, he’d be screwed.”
Indifference, resilience and ambivalence
Another segment of unvaccinated people obscured by the “hesitant” label are the “vaccine indifferent.” For various reasons, they remain relatively untouched[21] by the pandemic: COVID-19 just isn’t on their radar. This might include people who are self-employed or working under the table, people living in rural and remote places, and those whose children are not in the public school system.
Such people thus are not consistently connected to COVID-19-related information. This is particularly true if they forego social or news media and socialize with others who do the same, and if there are significant language barriers.
 CommuniVax researchers Sarah Song and Grecia Guerrero talk with potential participants outside a grocery store in June.
Diego Ceballos/CommuniVax, CC BY-ND[22]
CommuniVax researchers Sarah Song and Grecia Guerrero talk with potential participants outside a grocery store in June.
Diego Ceballos/CommuniVax, CC BY-ND[22]
We also learned that, among some of our participants, the initial messaging about prioritizing high-risk groups backfired[23], leaving some under 65 and in relatively good health with the impression it wasn’t necessary for them to get the vaccine. Without incentives – travel plans, being accepted to a college or having an employer that mandates vaccination – inertia carries the day.
The indifferent are not against vaccination. Rather, “if it ain’t broke, don’t fix it” and “you do you” tend to typify their views. As Jose from Idaho reported, “I’m not worried because I’ve always taken care of myself.”
We also saw a modified form of indifference in those who believed that the protective steps they already were taking would be enough to keep them COVID-19-free. A janitor said, “I am an essential worker… So from the beginning we took … all the precautions … face masks, taking [social] distance [and using] natural medicines and vitamins for the immune system.” He had, indeed, so far avoided contracting COVID-19.
The view of vaccines as not immediately necessary is magnified among some Latino people by the cultural value placed on the need to endure – “aguantar” in Spanish — to bear up, push through and avoid complaining about daily struggles. This perspective can be seen in many immigrant or impoverished populations, where getting sick or injured can be a precursor[24] to household ruin through job loss and exorbitant, unpayable medical bills.
Yet another dynamic we learned of is what we term “vaccine ambivalence.” Some participants who view COVID-19 as a significant health threat believe the vaccine poses an equivalent risk. We saw this particularly among African Americans in Alabama – not necessarily surprising given that the health care system has not always had these communities’[25] best interests[26] at heart. The perceived conundrum leaves people stuck on the fence. Given the legacy of unequal treatment[27] in communities of color, when balancing the “known” of COVID-19 against the unknown of vaccination, their inaction may seem reasonable – especially when coupled with mask-wearing and social distancing.
Attending to blind spots
At this point in the pandemic, those with the means and will to get vaccinated have done so. Providing viable counternarratives to misinformation[28] can help bring more people on board. But continuing to focus solely on individual mistrustfulness toward vaccines or so-called hesitancy obscures the other complex reasons people have for being wary of the system and bypassing vaccination.
[Over 100,000 readers rely on The Conversation’s newsletter to understand the world. Sign up today[29].]
Moreover, an overly narrow focus on the vaccine leaves a lot outside the frame. A wider view reveals that the problems leading to inequitable vaccination coverage are the same structural problems that have, historically, prevented people of color from having a fair shot[30] at good health and economic outcomes to begin with – problems that even a 100% vaccination rate cannot resolve.
References
- ^ nearly two-thirds (covid.cdc.gov)
- ^ lower on average among non-white people (covid.cdc.gov)
- ^ relatively lower vaccination rates in communities of color (covid.cdc.gov)
- ^ social factors (www.kff.org)
- ^ As medical (www.isu.edu)
- ^ anthropologists (scholar.google.com)
- ^ we take (anthropology.ua.edu)
- ^ CommuniVax (www.communivax.org)
- ^ national initiative to improve vaccine equity (www.communivax.org)
- ^ array of health inequities (www.nytimes.com)
- ^ combination of factors (www.cdc.gov)
- ^ disease severity (www.cdc.gov)
- ^ COVID-19-related trauma (theconversation.com)
- ^ 84% as of July 6, 2021 (www.sandiegocounty.gov)
- ^ well documented challenges (doi.org)
- ^ Johnson & Johnson vaccines promoted in their communities (www.cnbc.com)
- ^ Tom Brenner/Pool/AFP via Getty Images (www.gettyimages.com)
- ^ providers’ attitudes towards vaccines matter too (www.aafp.org)
- ^ can have downstream effects (doi.org)
- ^ current laws (www.boundless.com)
- ^ remain relatively untouched (doi.org)
- ^ CC BY-ND (creativecommons.org)
- ^ prioritizing high-risk groups backfired (www.washingtonpost.com)
- ^ can be a precursor (www.npr.org)
- ^ these communities’ (doi.org)
- ^ best interests (doi.org)
- ^ legacy of unequal treatment (doi.org)
- ^ counternarratives to misinformation (doi.org)
- ^ Sign up today (theconversation.com)
- ^ having a fair shot (www.cdc.gov)






















