A medical moonshot would help fix inequality in American health care
- Written by: Dana Goldman, Leonard D. Schaeffer Chair and Distinguished Professor of Public Policy, Pharmacy, and Economics, University of Southern California
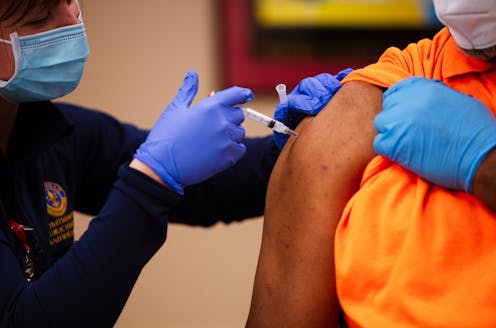
COVID-19 has put the American health care system’s deeply entrenched inequities into high relief. The social, economic and political structures that predated the pandemic’s public health crisis and resulting recession have meant that Black and Latino people are more likely than white people to be exposed to, hospitalized for and die from COVID-19[1]. But Black and Latino people also died at higher rates than whites from non-COVID-19 causes in 2020[2], underscoring the harm of delays in medical care generally.
Simply put, inequity kills.
As a health economist[3], an expert in social determinants of health[4] and a professor of health policy[5], we have seen the evidence that new medical interventions can serve as a great leveler and help change the trajectory of health disparities in the United States. A concerted national effort to develop cures or enhanced treatments for conditions that disproportionately affect communities of color – such as high blood pressure, diabetes and obesity – would benefit all patients, while narrowing racial and ethnic disparities.
How innovation can transform health outcomes
Medical breakthroughs, as well as new ways of delivering existing treatments, can help advance health equity. How? Improved testing, diagnosis and treatment can help identify those who need care and can get them better care. But innovations don’t do that on their own.
Hypertension provides a good example. Breakthroughs in treatment over the past few decades – including antihypertensive medications, cholesterol-lowering drugs and heart surgery – helped decrease overall deaths in the U.S. from heart disease by 47% over two decades[6]. But mortality among Black Americans is improving at a slower rate[7] than for their white counterparts, even though Black Americans are more likely to develop serious hypertension and have worse health outcomes – in part because they are less likely to receive[8] key diagnostic tests and treatments.
The story has been somewhat different with HIV. Since the first wave of complex drug treatments in the 1990s, significant innovations – from combination treatments to single-tablet regimens to pre-exposure preventive treatment – life expectancy has increased and infection rates are down. People on single-tablet regimens[9], for instance, have been better able to maintain treatment regimens, leading to improved viral suppression and fewer hospitalizations[10].
These simplified regimens help close disparities in HIV infection and treatment among people of color, who due to historic inequities found it more difficult to adhere to the earlier, more complex HIV treatment regimens[11]. Improving outcomes for this population was a key component of the national strategy[12] to end the HIV epidemic.
Linking innovation to equity
New COVID-19 vaccines promise similar benefits. Single-dose administration, for example, eliminates the scheduling, transportation and child care needed for a second dose, making it ideal for hard-to-reach populations[13]. Community leaders in Washington, D.C., for example, used single-dose jabs at a mobile vaccination clinics[14] stationed in African American churches.
Similar innovations could help improve management of asthma or diabetes[15], which both afflict nonwhite people at higher rates[16] than white Americans. Or make screenings for cancer and other chronic conditions more accessible, promoting earlier detection in another arena where significant health disparities exist.
Innovation is also key to addressing the health care needs of older adults, including older adults of color. The pandemic’s disproportionate impact on those living and working in long-term care facilities[17] has exposed the need to assist all health care workers, not just doctors and nurses. Beyond these measures, technological advances – from telemedicine to remote monitoring to therapeutic robots – have the potential to promote healthy, successful aging and improve disparities.
Innovation is just part of the solution
The White House and the National Institutes of Health[18] have proposed a new public-private initiative to improve health. It would be modeled on the successful DARPA effort by the Department of Defense[19], which led to such technologies as the internet and GPS. To achieve equal access to health care, this initiative needs to work on not just developing new technologies, but also ensuring equal access.
It may not seem like much to simplify the steps in a treatment regimen or reduce the necessary number of visits to a doctor – but these can make a difference in people’s lives.
We also need more inclusive research designs. Including patients of color in clinical trials[20] to test new drugs is vital to learn how well new interventions work across the entire population.
Communication strategies tailored to and respectful of marginalized communities[21] would reach them with messages that resonate with their concerns.
[You’re smart and curious about the world. So are The Conversation’s authors and editors. You can read us daily by subscribing to our newsletter[22].]
Medical advances are often costly as well. The promise of innovation can be realized only if new technologies are appropriately reimbursed by Medicare and Medicaid – the U.S.‘s key public payers. So any health moonshot must also eliminate financial and other barriers to accessing new innovations.
Many factors contribute to health disparities. A systemic, multifaceted and trustworthy approach to closing them should not overlook the potential of new medical innovations in the fight to end health disparities for patients of color. Lives and livelihoods depend on it.
References
- ^ to be exposed to, hospitalized for and die from COVID-19 (www.cdc.gov)
- ^ died at higher rates than whites from non-COVID-19 causes in 2020 (www.cdc.gov)
- ^ health economist (scholar.google.com)
- ^ social determinants of health (scholar.google.com)
- ^ professor of health policy (www.aging.columbia.edu)
- ^ deaths in the U.S. from heart disease by 47% over two decades (dx.doi.org)
- ^ is improving at a slower rate (www.cdc.gov)
- ^ they are less likely to receive (doi.org)
- ^ single-tablet regimens (doi.org)
- ^ leading to improved viral suppression and fewer hospitalizations (doi.org)
- ^ more difficult to adhere to the earlier, more complex HIV treatment regimens (dx.doi.org)
- ^ the national strategy (www.hiv.gov)
- ^ hard-to-reach populations (theconversation.com)
- ^ mobile vaccination clinics (www.wusa9.com)
- ^ improve management of asthma or diabetes (doi.org)
- ^ at higher rates (www.lung.org)
- ^ living and working in long-term care facilities (www.kff.org)
- ^ White House and the National Institutes of Health (dx.doi.org)
- ^ DARPA effort by the Department of Defense (www.darpa.mil)
- ^ patients of color in clinical trials (dx.doi.org)
- ^ tailored to and respectful of marginalized communities (www.kqed.org)
- ^ You can read us daily by subscribing to our newsletter (theconversation.com)

























